We're growing! Find your way while visiting the ACH campus. Learn more >
We're growing! Find your way while visiting the ACH campus. Learn more >
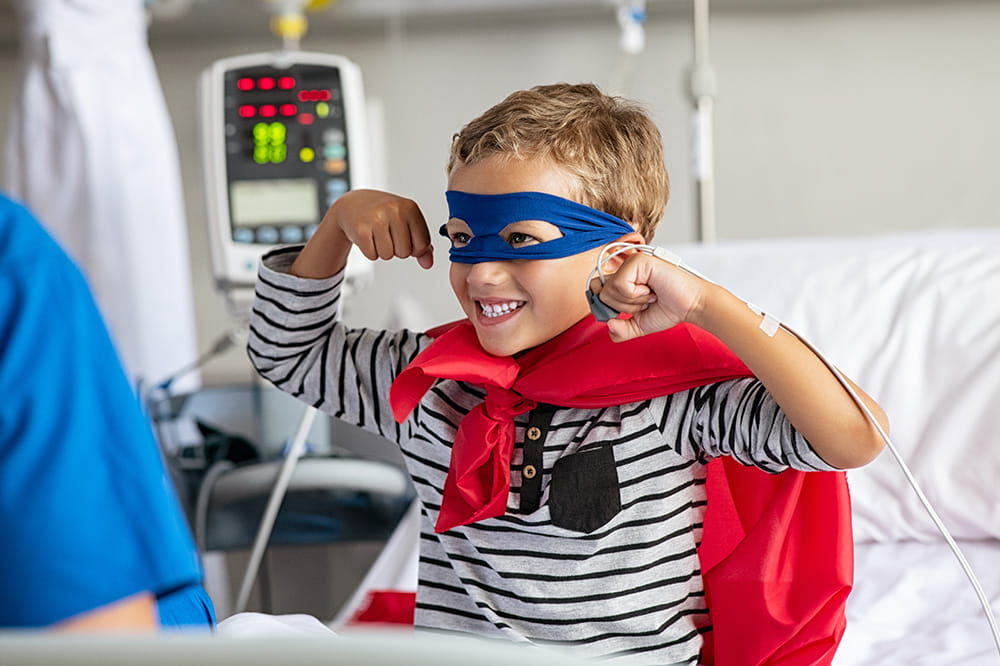
Arkansas Children's provides right-sized care for your child. U.S. News & World Report has ranked Arkansas Children's in seven specialties for 2023-2024.

Sign up online to quickly and easily manage your child's medical information and connect with us whenever you need.
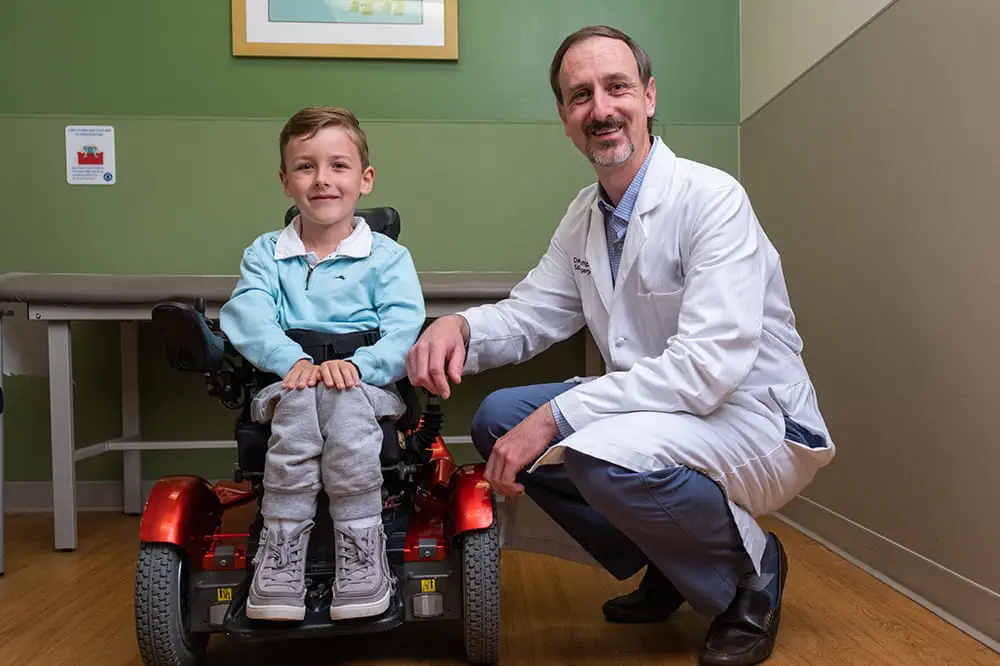
We're focused on improving child health through exceptional patient care, groundbreaking research, continuing education, and outreach and prevention.

Our ERs are staffed 24/7 with doctors, nurses and staff who know kids best – all trained to deliver right-sized care for your child in a safe environment.

Arkansas Children's provides right-sized care for your child. U.S. News & World Report has ranked Arkansas Children's in seven specialties for 2023-2024.

Find health tips, patient stories, and news you can use to champion children.

Our flu resources and education information help parents and families provide effective care at home.

We are dedicated to caring for children, allowing us to uniquely shape the landscape of pediatric care in Arkansas.

Our researchers are driven by their limitless curiosity to discover new and better ways to make these children better today and healthier tomorrow.

We're focused on improving child health through exceptional patient care, groundbreaking research, continuing education, and outreach and prevention.
Then we're looking for you! Work at a place where you can change lives...including your own.

When you give to Arkansas Children's, you help deliver on our promise of a better today and a healthier tomorrow for the children of Arkansas and beyond

The gift of time is one of the most precious gifts you can give. You can make a difference in the life of a sick child.

Support and participate in this advocacy effort on behalf of Arkansas’ youth and our organization.

Scientific discoveries lead us to new and better ways to care for childlren.

Scientific discoveries lead us to new and better ways to care for childlren.

Scientific discoveries lead us to new and better ways to care for childlren.

Scientific discoveries lead us to new and better ways to care for childlren.

Scientific discoveries lead us to new and better ways to care for childlren.

Scientific discoveries lead us to new and better ways to care for childlren.
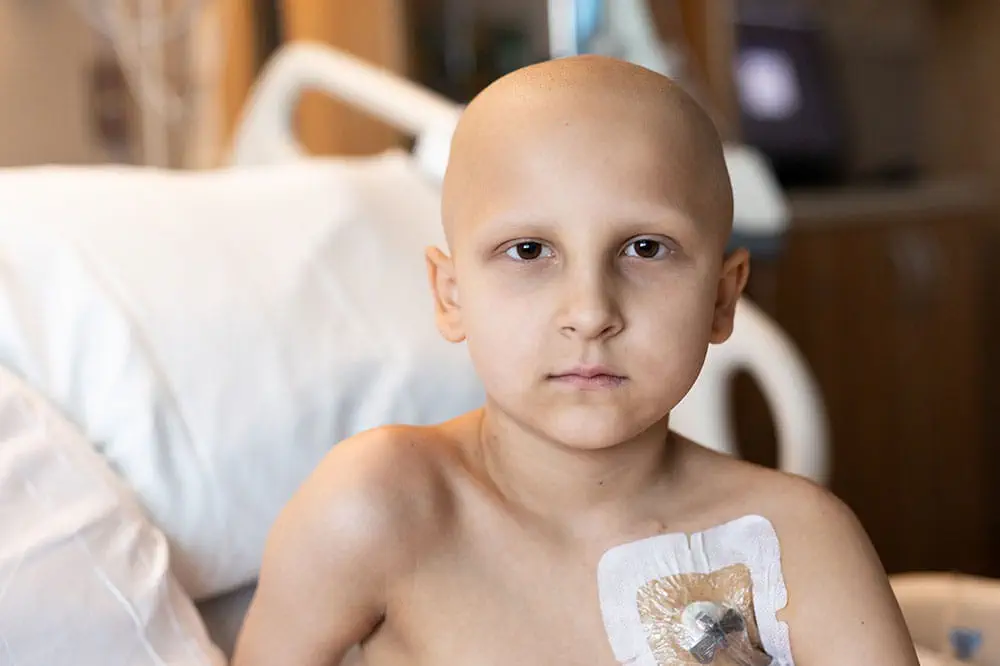
When you give to Arkansas Children’s, you help deliver on our promise of a better today and a healthier tomorrow for the children of Arkansas and beyond.

Your volunteer efforts are very important to Arkansas Children's. Consider additional ways to help our patients and families.

There are many ways to get involved to champion children statewide.

The generosity of our supporters allows Arkansas Children's to deliver on our promise of making children better today and a healthier tomorrow.

Read and watch heart-warming, inspirational stories from the patients of Arkansas Children’s.
Manage your child's medical information and connect with your Arkansas Children's medical team online.
Login Sign upArkansas Children's Hospital
General Information 501-364-1100
Arkansas Children's Northwest
General Information 479-725-6800
Getting a good night’s sleep is incredibly important for your child’s health and well-being. Sleep problems such as sleep apnea, excessive daytime sleepiness, narcolepsy, and behavioral sleep problems are common and can seriously affect your child’s general health, academic functioning, behavior, and mood. The Sleep Disorders Center provides comprehensive clinical evaluation, diagnostic testing, treatment and follow-up for a wide spectrum of sleep-related disorders in children and adolescents. The Pediatric Sleep Disorders Center’s goal is to find the best solutions to your child’s sleep issues and to help them sleep better. The center offers state-of-the-art technology designed to evaluate sleep physiology and treat sleep-related disordered breathing.
ACH is one of only a few pediatric hospitals in the nation to receive full-service accreditation from the Association of Sleep Disorders Centers (American Academy of Sleep Medicine). Nationally accredited by the American Academy of Sleep Medicine (AASM), we offer the highest standard of care, commitment to quality services and dedication to our patients
The Sleep Disorders Lab only AASM accredited pediatric sleep disorders lab in the state; offers state-of-the-art technology designed to evaluate sleep physiology, diagnose sleep disorders and guide treatment of sleep-related disordered breathing.
Getting a good night’s sleep is incredibly important for your child’s health and well-being. Sleep is vital for learning and memory and lack of sleep impacts a child’s health negatively. At Arkansas Children's we work to make your child healthier tomorrow by treating sleep problems such as sleep apnea, excessive daytime sleepiness, narcolepsy, and behavioral sleep problems are common and can seriously affect your child’s general health, academic functioning, behavior, and mood.
Obstructive sleep apnea (OSA) is a condition where breathing is affected during sleep due to obstruction of the upper airway. This occurs during sleep because the muscles in the airway relax and the airway partially closes.
Excessive sleepiness is a symptom caused by poor sleep habits, an irregular sleep schedule, obstructive sleep apnea, medications, and other underlying medical conditions.
Narcolepsy and Idiopathic Hypersomnolence are disorders of excessive sleep (hypersomnolence). Both of these problems may be evaluated with a polysomnogram to rule out other sleep problems followed by a multiple sleep latency test (MSLT) which evaluates the sleepiness of the child. Treatments may consist of individualized medication management, scheduled naps and modifications of work/school schedules.
Parasomnias are a group of sleep disorders that involve undesirable physical events or experiences that occur while falling asleep, during sleep, or while waking up from sleep.
Periodic limb movement disorder (PLMD) are repetitive limb movements that occur every few seconds during sleep.
Restless legs syndrome (RLS) is a movement disorder characterized by an uncomfortable sensation or irresistible urge to move your legs that occurs while awake and relaxing.
Infants, children and adolescents may develop bad sleep habits surrounding bedtime. These may include delayed bedtimes, difficulty falling asleep, frequent arousals/waking during the night, and difficulty waking up in the morning.
The Sleep Disorders Center Team at Arkansas Children's takes a comprehensive, team approach customized to treating your child's care. Choose the Sleep Disorders Center Team at Arkansas Children's, where you'll be treated by some of the best available.
Pulmonology (Sleep Disorders)
Little Rock, Springdale
Pulmonology (Sleep Disorders)
Little Rock, Springdale
An Arkansas Children's Podcast is about the people, places, and programs of Arkansas Children's. Podcasts are available monthly on Apple Podcasts and Google Podcasts.
Behavioral modification therapy can improve your child’s sleep by changing their behavior before bedtime as well as changing things that keep your child from falling asleep or staying asleep. It helps your child develop habits that promote a healthy pattern of sleep.
An effective therapy to treat obstructive sleep apneas (OSA) and sleep-disordered breathing in children and adolescents is with non-invasive positive airway pressure (PAP). PAP therapy involves the delivery of room air by way of a bedside machine that delivers a stream of air to the child’s airway using an oral or nasal mask. This stream of air prevents airway collapse.
The term “sleep hygiene” refers to healthy sleep habits that can improve your ability to fall asleep and stay asleep. Sleep hygiene is a variety of good sleep habits that are necessary to have quality nighttime sleep and full daytime alertness.
Actigraphy is worn like a watch on the wrist and is used to assess cycles of activity and rest over several days or weeks. It measures activity through light and movement.
Our Sleep Clinic is available by physician referral. An outpatient clinic visit consists of a comprehensive evaluation which may include a physical exam, lab tests and x-rays.
The Sleep Disorders Center may use the Maintenance of Wakefulness Test (MWT) to measure how alert you are during the day.
The multiple sleep latency test is used to measure the tendency to fall asleep during the daytime after a good night’s sleep.
An overnight polysomnogram (PSG), also known as a sleep study, is used to diagnose sleep disorders. The test is available upon request from the provider and most polysomnograms are performed in the sleep lab.
Our chaplains are on staff to assist all patients and families from any faith background with religious and spiritual needs.
Child Life reduces stress and promotes positive coping using developmentally appropriate preparation, education, and play at Arkansas Children's.
Arkansas Children's offers on-site dining, shuttle services, and gift shops, as well as discounted hotels and rv parks nearby.
Untreated sleep apnea in pediatric patients can negatively impact health and learning. Lean more about Arkansas Children’s treats central and obstructive sleep apnea.
Dr. Supriya Jambhekar, one of our experts on sleep disorders, talks about why sleep is important and how much sleep children need.
Baby boys, young boys and teenagers, can have a unique set of urological challenges that generally have no lasting effects if treated early
Starting a heart-healthy routine with your child while they are young creates building blocks for a hearty future.
Arkansas Children's offers seven tips to a better bedtime routine.
Learn about how much sleep you child needs, how to set a routine, sleep tips, and learn about sleep disorders. Pediatric sleep disorders expert Dr. Jambhekar joins us to talk All About Sleep!
Parker sees an ACH pediatric asthma specialist via telehealth at the ACH Jonesboro Clinic. Watch this video to learn how to keep asthma under control using telehealth.
Our app is designed to be your "go-to" for managing your child's health day or night.
Arkansas Children's has an online bill pay system to pay your bill for visits and admissions.
Manage your child's medical information and connect with your Arkansas Children's medical team anytime online!
Log in to MyChartAccess the information and tools you need to stay connected with Arkansas Children's quickly.
Arkansas Children's offers translation assistance to the hearing impaired as well as non-English speaking patients and families.